It was nerve wrecking to see my little one (No.4) went out of breathe from coughing. I will share my first-time experience admitting one of my children to a hospital.
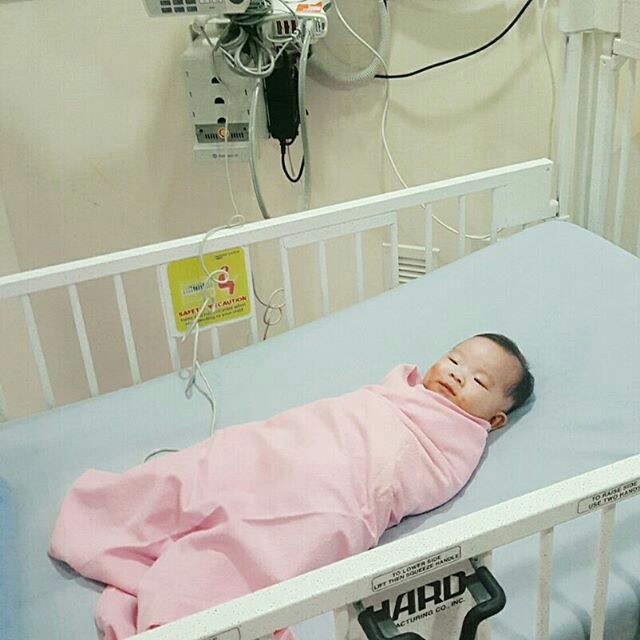
It developed from a mild cough…
We found it odd to hear a 10-week old baby coughing. By the time she was 12-week old, she coughed so intensely that she vomited half of the time. She had gradually lost her appetite too.
One day, she coughed so hard a couple of times that she became breathless and her face turned red. That was the last straw. We decided it was necessary to send her to KKH for a check. While the average wait at A&E for a non-emergency case is about 4 hours, our 3-month old baby was given priority and we waited for less than 30 minutes after the nurse at the triage gave our baby an initial assessment.
The paediatrician decided that our baby should be admitted for future observations in consideration of the following:-
-
loss of appetite
-
signs of choking
-
the risk of pertussis
What is Pertussis?
According to MOH, pertussis is a whooping cough and is a highly contagious respiratory disease. This is caused by a type of bacteria known as Bordetella. It is air-borne and can be fatal in the case of an infant. In Singapore, most babies are vaccinated against pertussis before they reach 5 months old. Our baby was sent to an isolation ward while waiting for her swab test result.
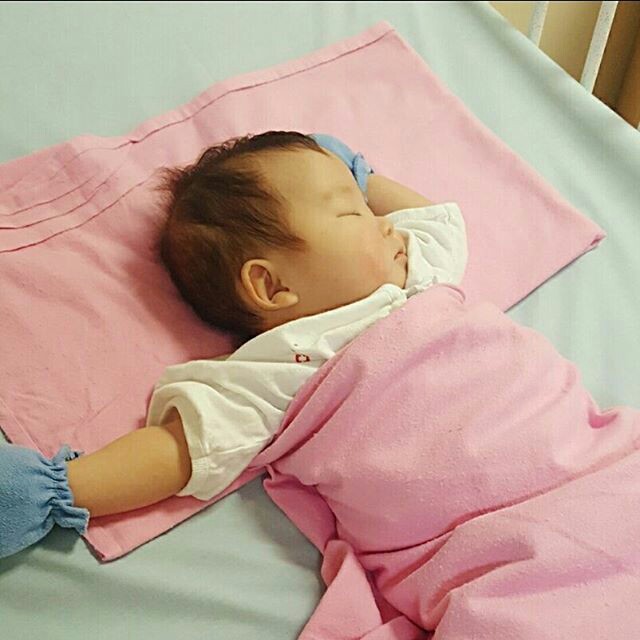
Loss of Appetite
By the second day of admission, No.4 could neither latch nor be bottle-fed. Her near total loss of appetite was as a result of her cough and running nose. Babies at this age breathe through their nose and could only counteract their blocked nose by crying if they need to catch their breath.
I was so worried and loss, and yet was grateful that we were actually staying in the hospital. The nurses provided me with professional support and comfort.
What did the nurses do?
-
Regular use of nasal spray and aspirator to clear out the baby’s mucus. We can do this at home too

-
Inserted a gavage tube into the baby’s stomach to facilitate tube feeding.

It was heartbreaking for us to see a tube hanging out from our infant’s nose.
No, it was not pertussis.
By Day 3, our little baby was transferred to a normal ward after her swab test confirmed that she was not infected with pertussis.
Then what is it? The hospital did another test for 20 other types of infection but did not have any conclusion. We could have persisted to go for more tests as there are 300+ viruses which can be tested for. However, as the baby has not developed any fever nor any other life-threatening symptom, the doctors did not suggest to pursue further.
Doctors encouraged us to give our baby to take in more breast milk as it contains antibodies to help baby recover sooner. That freaked me out for a few days as I did not have enough to supply her 100%. I spent those few days obsessing with my milk quantity and zealously pumping every 3 hours. See my post here on how I managed to stay sane despite low milk supply.
Our Mini Feeding Saga
By Day 4, the pediatrician-in-charge recommended for baby to be discharged. She changed her mind after I whined about baby’s feeding ability as her latch remained poor and she rejected milk bottle. More than often, we had to resort to tube feeding.
By Day 5, the pediatrician instructed the nurses to remove the tube from our baby. She was of the view that the tube inhibited baby’s feeding ability. She instructed us to monitor baby’s intake amount. As long as she can take in 300mil by herself, she is ready to be discharged. All this while, I expressed my milk so that we knew exactly how much baby is drinking.
Throughout the hospital stay, we switched her milk bottle a couple of times. The nurses advised that No.4 might find her NUK teat difficult to suck while having a blocked nose. Thus, from NUK, we switched to Pigeon and then to a disposable teat meant for premature babies. No.4 was finally sucking.

Day 6, our baby was finally discharged. We bought new Medela teats which are narrower that the NUK ones. No.4 finds no difficulty sucking and we went home with a piece of mind.
Related post: we bought a nebulizer for our babies’ use.
Our Hospital Bill
We are very fortunate to be fully covered by health insurance from a private insurer. In fact, our underwriting was approved just 2 weeks before admission!
As of now…
Nearly one month after discharge, our little ones are still coughing and remain under treatment. We went back to the doctor when No.3 ran a fever coupled with a cough. Apparently, the medical staffs observed that many babies below 6 months are coughing recently and many suffered from bronchitis.
My key takeaway from this experience:
-
Insurance is a must-have,
-
Get vaccinated on time,
-
you must bring your baby to see a doctor if your newborn has the following symptoms:
-
fever above 38.5ºC
-
loss of appetite
-
signs of choking.
Keen to hear more from me? You can subscribe to my blog via email or like my facebook page.
-


